

During pregnancy hormonal changes can have effects on the gums and teeth, so at this stage, we must take special care with our oral health. The secretion of hormones such as estrogen increases 30 times more than normal and progesterone 10, compared to what happens in the normal sexual cycle of women. In the second month of gestation the inflammatory symptoms and signs begin, which are maintained or increased during the second trimester, peak at the eighth month, descend during the last month, and remit after childbirth.
The most frequent and marked changes lie on the gingival tissue (gums), giving rise to the so-called pregnancy gingivitis, a condition characterized by an enlarged gum, red and bleeding easily; also, the granuloma of pregnancy (approximately 1 in 10 pregnant women with gingivitis suffers this disease), which is another alteration of gingival tissue in the presence of local irritants. Despite all these vascular changes, plaque remains the fundamental factor in the development of gingivitis.
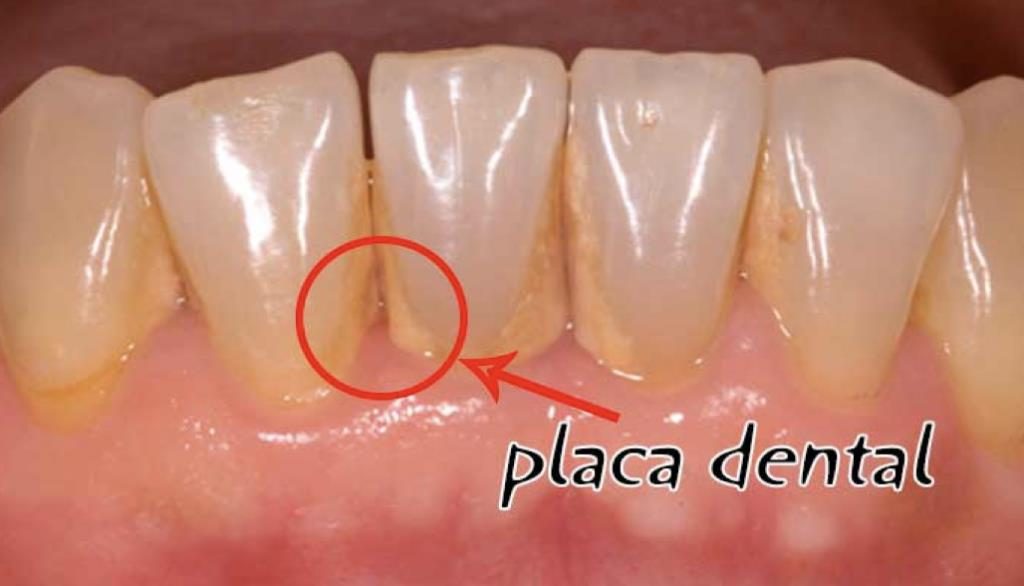
Dental plaque is an accumulation of microorganisms that adhere to the walls of the teeth, and that survive by feeding on the substrates they find in the mouth and when they persist they cause caries, gingivitis or periodontal diseases.
Multiple scientific evidence indicates that poor hygiene before and during pregnancy is the main predisposing factor to the above-mentioned pathologies. Studies suggest that up to 18% of preterm births can be justified by the presence of periodontal disease and it is considered that between 30% and 50% of these are caused by infections.
On the other hand, pre-eclampsia (the joint appearance of arterial hypertension and proteins in the urine) is one of the main causes of maternal and neonatal mortality and morbidity. In Spain, this relationship is considered to exist between 1% and 2% of pregnancies. Women with periodontal disease have 5 times more risk of suffering preeclampsia during pregnancy than women who are healthy gingivally, 4 to 7% of suffering a premature birth and is one of the main causes of births weighing less than 2.5 kg. Therefore, we must know that the best treatment for gum problems, as well as the greater presence of caries, is preventive treatment.
Although these physiological changes occur in all pregnant women, not all of them have the alterations described. This is due, in part, to the individual genetic predisposition to suffer or not certain diseases, as well as to the oral hygiene carried out daily by each of the pregnant women.
FAQS:
– DURING PREGNANCY, DOES THE BABY STEAL THE MOTHER’S CALCIUM AND LOSE TEETH DUE TO THE DECALCIFICATION?
The first thing is to understand that the teeth are attached to the jaw bone (mandible) by the periodontal ligament, which is responsible for holding the tooth inside the gum.
The organism in the state of gestation produces a hormone called relaxin, whose function is to relax the joints of the pregnant woman to facilitate childbirth. Some studies suggest that this hormone can also act in the periodontal ligament causing a slight dental mobility that facilitates the entry of food debris and that the plaque dentobacterial is deposited between the gum and the tooth, causing inflammation of these. This dental mobility caused by this reason does not cause loss of dental insertion, and does not require treatment, remitting in the postpartum.
Pregnancy does not cause bone loss. The total amounts of calcium and phosphorus needed by the fetus during pregnancy represent only 1/50 of the amount present in the maternal bones. Therefore, the maternal organism suffers very little in this respect. Virtually everywhere in the world, there is a mistaken belief that pregnancy costs a pregnant woman a tooth or more because the baby steals the mother’s calcium. What we can affirm is that during the state of gestation there are changes in the oral tissues and changes of habits that can initiate oral diseases or aggravate the existing ones, increasing the carious activity, nevertheless, studies carried out have demonstrated that, unlike the skeleton, in this state there is no demineralization of the teeth. The enamel has a very slow mineral exchange, so it keeps its mineral content all its life. Much of what happens in the enamel takes place by replacement of minerals with those of saliva and not by decreased calcium. In this sense, it is stated that calcium is not extracted from dental tissue, even though the requirements of this element are increased by 33 % in comparison with non-pregnant women.
– “DO WE HAVE A GREATER PREDISPOSITION TO TOOTH DECAY?”
The first stage in the development of caries is plaque, which as we have said is inhabited by many bacteria that feed on carbohydrates or sugars found in our mouth, and from here produce acids, particularly lactic acid and proteolytic enzymes. Acids are the main cause of tooth decay. Each time sugar is ingested, the acids attack the tooth enamel for approximately 20 minutes, so the acid attack is proportional to the time there is sugar, which explains that it is the frequency and not the amount of sugar ingested that causes tooth decay. If you cannot brush your teeth after a meal, we advise exceptionally, chewing sugar-free gum, to neutralize the acids. Brushing is irreplaceable for daily hygiene.
During gestation, women are more vulnerable to dental caries. Changes in salivary production, oral flora, diet, among others, are factors capable of producing it. During this period, the salivary composition is altered, the salivary pH decreases and the ability to regulate the acids produced by bacteria, which makes the oral environment favorable for the development of these.
On the other hand, we cannot ignore that, during this stage, some women modify their eating habits (sweet food cravings) and lifestyles (deficiency of brushing due to the nausea produced by the practice of this habit), all of which contributes to the accumulation of dentobacterial plaque adhered to the surface of the tooth. With all these factors interacting with each other, the dental caries succeeds in establishing itself, and in some cases produces dental mortality the infection reaches the dental nerve, we feel pain and we must endodontize the piece.
“DOES VOMITING DURING PREGNANCY DAMAGE TEETH?”
Excessive vomiting (due to morning sickness), as well as gastric acids, can cause dental erosion, lead to a loss of minerals from the teeth and encourage tooth decay. The gums can also be affected. The dentist should be informed of this phenomenon by applying fluoride to the teeth or recommending a fluoride paste and mouthwash to prevent this problem. We recommend that as soon as you vomit, do not brush your teeth, as we will drag the remains of acid throughout the mouth, favoring dental wear. It is best to rinse your mouth well after vomiting to remove any remaining acid.
“WHAT SHOULD I DO IF I SUFFER FROM DENTAL DISEASE DURING PREGNANCY?
Dental treatment during the first and third trimesters should be kept to a minimum. They are trimesters where it is recommended to go to the dentist to control the plaque and the general state of the mouth. The second trimester of pregnancy is the safest time to provide regular dental care. The most important thing is to avoid active disease. The elimination of any focus of infection should be done before the pregnancy itself, whenever possible, but if it should arise, it should be addressed with appropriate measures in any period of pregnancy.
If tooth decay is established, curative treatment is required, which should not only be seen from the maternal point of view, but also from the consequences it may have for the future baby. A study in Finland showed that those mothers who received treatment for dental caries during pregnancy, unlike those who received no treatment, had children with low incidence of dental caries during the temporary dentition. This result demonstrates that dental treatment during pregnancy can affect the development of caries in the child’s temporary dentition, possibly by transmission of immune mechanisms through the placental canal.
– IS IT SAFE TO HAVE DENTAL TREATMENT UNDER ANESTHESIA?”.
Lidocaine (anesthesia used in dental treatment) is safe for both you and your baby.
An August 2015 study in the ADA Journal followed a group of pregnant women who had interventions using anesthesia such as lidocaine injections and a group who did not. According to the study, these treatments are safe because they make no difference in the rate of miscarriage, birth defects, prematurity or weight of the baby. “Our study did not identify any evidence that dental treatment with anesthesia is harmful in pregnancy,” stated study author Dr. Hagai. “Our goal was to determine if there was a significant risk associated with anesthesia treatment and pregnancy outcomes. We found no such risk.
-IS CHLORHEXIDINE SAFE FOR THE TREATMENT OF PERIODONTAL DISEASE/GINGIVITIS?”.
Medication use during pregnancy should be fully controlled by the referring physician. Specifically, the use of chlorhexidine in any of its forms (paste, gel or rinse) is completely safe and can be used during pregnancy if necessary. It does not have synthetic absorption and its antibacterial effects will be restricted to the mouth.
-ARE INTRA-ORAL X-RAYS SAFE DURING PREGNANCY?”
Yes, dental x-rays are safe during pregnancy. Routine check-up x-rays should be avoided during pregnancy. However, in the event of a dental emergency they may be necessary, with due protection. Dental x-rays are not contraindicated in pregnancy, because the radiation that is exposed to the fetus is minimal. Therefore, there is no risk of teratogenesis (congenital defect during gestation) due to exposure to this type of x-ray.
Your dentist or hygienist will cover you with a protective apron that minimizes exposure of the abdomen. For this reason, it is extremely important that before taking the x-ray it is stated that you are pregnant so that all the necessary precautions are taken, since x-rays will only be taken when it is extremely necessary. In all patients, and especially in pregnant patients, the indication of the x-ray is done considering the risk of exposure and considering the benefit it can have to facilitate the diagnosis.
“WHEN DO I START BRUSHING MY BABY’S TEETH?
Brushing teeth with fluoride toothpaste is recommended at least twice a day from the first tooth eruption. In children under 2 years with a toothpaste of 1,000 ppm (parts per million) of fluoride “scraped” onto the brush, i.e. the total amount of toothpaste should be the size of a grain of rice. Between 2-6 years, paste 1000-1450 ppm and the amount the size of a pea. Above 6 years, paste with 1,450 ppm of fluorine and the amount of 1 – 2 cm on the brush. The mouthwashes from 6 years, by risk that they ingest it. They must spit it out completely. From this age, the first visit to the pediatric dentist is recommended, since, from this age, they begin to change the milk teeth for the definitive ones. In any case, whenever you notice oral lesions, cavities in baby teeth or you have doubts about how to take care of your child’s oral health, do not wait until you are 6 years old, go to your pediatrician.
CONCLUSIONS ABOUT ORAL CARE IN PREGNANCY:

The most important goal is to establish a healthy oral environment and achieve the highest level of oral hygiene.
All gestational women are prone to changes in their bodies, but this does not mean that all of them have the alterations described here implicitly. A good control of the brushing together with an increasing care of the oral hygiene, diet, and the periodic oral examination, will contribute to diminish or to control these alterations, reason why we can conclude that the state of gestation modifies the buccal conditions and affects of this form in the buccal health, and that the tooth, the periodontal tissues and the buccal mucosa are the direct targets that can be affected by this motive.
The most important thing to prevent caries and gingivitis is to carry out a meticulous tooth brushing with fluoride paste at least twice a day and to carry out interdental hygiene at least once a day. In women with a greater predisposition to caries and gum disease, a fluoride mouthwash and antimicrobial agents should be used.
We recommend a minimum of one visit to your dentist during your pregnancy who will control the plaque to minimize gum irritation. The elimination of tartar, oral cleaning, the application of fluoride to prevent cavities and root scraping and smoothing is recommended and can be done when necessary.